Does Medicare Cover Acupuncture For Allergies
Acupuncture is sometimes used to treat allergies. Some Medicare Advantage plans help cover acupuncture even though it is considered alternative medicine and is not covered by Original Medicare.
Note: coverage and costs will vary depending on the Medicare Advantage plan youre enrolled in, and not every Medicare Advantage plan covers acupuncture.
A licensed insurance agent can help you compare Medicare Advantage plans in your area and get you enrolled in a plan that works for you.
Find Medicare Advantage plans in your area
Or call 1-800-557-6059TTY Users: 711 to speak with a licensed insurance agent. We accept calls 24/7!
Get the Scoop!
Join our email series to receive your Medicare guide and the latest information about Medicare and Medicare Advantage.
When Should I See A Doctor Because Of The Side Effects I Experience From Shingrix
In clinical trials, Shingrix was not associated with serious adverse events. In fact, serious side effects from vaccines are extremely rare. For example, for every 1 million doses of a vaccine given, only one or two people may have a severe allergic reaction. Signs of an allergic reaction happen within minutes or hours after vaccination and include hives, swelling of the face and throat, difficulty breathing, a fast heartbeat, dizziness, or weakness. If you experience these or any other life-threatening symptoms, see a doctor right away.
Shingrix causes a strong response in your immune system, so it may produce short-term side effects more intense than you are used to from other vaccines. These side effects can be uncomfortable, but they are expected and usually go away on their own in 2 or 3 days.
One Allergy Test Alone Can Cost Anywhere From $275 To 350
Does insurance cover allergy shots. Yes, most allergy tests will be covered by health insurance, and the specialist administering the test will most likely be a network provider. Allergy shots may be cheaper. How much you can expect to pay out of pocket for allergy shots, including what people paid.
Allergy tests are considered part of the clinical diagnostic laboratory services category for medicare. The value of the measurement of fica toward the diagnosis of food allergy remains unproven and does not have a place in current clinical practice. Aetna covers immunotherapy for members with seasonal allergies.)
The lack of fda approval does mean that insurance will not cover allergy drops and patients will be responsible for the full cost. Allergy treatments may include allergy shots, medicine, and avoiding the substance that causes the allergic reaction. but not so much that i can switch up my routine. (your health insurance plan may cover allergy shots
If that is the case, the final allergy test cost will have more to do with the health insurers allowable cost for the specific test. Melissa began immunotherapy 10 years ago. You are allergic to only a few substances, and they are hard to avoid.
The cost of allergy shots for 131,493 people totaled $253,301,575. Avoiding allergens and using medicine do not control symptoms, or you have to take medicine all the time to control symptoms. A doctor has prescribed the shots.
Don’t Miss: What Allergy Medicine Is Stronger Than Zyrtec
Does Medicare Cover Allergy Testing And Shots
If allergy testing, allergy shots, or other allergy treatments are considered medically necessary, then Medicare Part B will most likely cover them. Medicare Advantage may cover more or less than what Medicare Part B does, so you will have to contact your plan provider to see what your coverage options are.
Read more below about how Medicare allergy testing coverage works.
Allergy Immunotherapy For The Treatment Of Allergic Rhino

The European Academy of Allergy and Clinical Immunology s Position paper on Allergen immunotherapy trials for allergic rhino-conjunctivitis stated that a standardized and globally harmonized method for analyzing the clinical effectiveness of allergen immunotherapy products in RCTs is needed. The EAACI Task Force highlighted the combined symptom and medication score as the primary end-point for future RCTs in AIT for allergic rhino-conjunctivitis.
Recommended Reading: Allergies Causing Nausea
Igg4 Testing For The Evaluation Of Allergy
The AAAAI stated that Dont perform unproven diagnostic tests, such as immunoglobulin G testing or an indiscriminate battery of immunoglobulin E tests, in the evaluation of allergy. Appropriate diagnosis and treatment of allergies requires specific IgE testing based on the patients clinical history. The use of other tests or methods to diagnose allergies is unproven and can lead to inappropriate diagnosis and treatment. Appropriate diagnosis and treatment is both cost effective and essential for optimal patient care.
Does Medicare Cover Allergies
July 2, 2021 / 2 min read / Written by Jason B.
If you have allergies, youre not alone.
- The Centers for Disease Control and Prevention notes that more than 50 million Americans suffer from allergies.
- An estimated 30% of adults and 40% of children are affected, estimates the American College of Allergy, Asthma & Immunology.
- Allergies are the sixth leading cause of chronic illness in the United States, according to the CDC.
- Allergies run up an estimated $18 billion annually in health-care costs, reports the CDC.
What are allergies?
Your immune system protects you from infections. According to the CDC, if your immune system overreacts to certain substances called allergens, this can produce allergies. They often cause you to sneeze or cough, or cause itching.
Allergies: what types are there?
There are many types of allergies. The Centers for Disease Control and Prevention lists asthma, eczema, hay fever, dermatitis, sinusitis, and conjunctivitis. National Institute of Allergy and Infectious Diseases adds allergies to food, mold, latex, insect stings, pet allergies, and drugs to the list.
Allergies: is there a cure?
Theres no cure for allergies, according to the Asthma and Allergy Foundation of America. But in many cases, the symptoms can be treated with prescription medications or allergy shots, notes the National Institutes of Health.
Allergies: does Medicare cover them?
NEW TO MEDICARE?
Read Also: Cetirizine For Allergic Rhinitis
When Does Medicare Part B Pay For Allergy Shots
Medicare does not have specific guidelines about how it covers allergy shots and allergy treatments. Coverage decisions are made on a case-by-case basis and may depend on the types of allergies you have and their severity.
If your doctor determines that an allergy shot is medically necessary, Medicare Part B or a Medicare Advantage plan may cover the cost of your shot.
A doctor may determine your allergy shots are medically necessary for one of the following reasons:
If Medicare covers your allergy shot, you will typically pay a 20% coinsurance or copay after you meet your annual Part B deductible, which is $203 in 2021.
All Medicare Advantage plans are required by law to provide at least the same minimum coverage as Medicare Part A and B, so a Medicare Advantage plan will also cover at least 80% of the cost of your allergy shots if your doctor says they are medically necessary.
Compare Medicare Advantage plans online to find the best plan for you. You may be able to find a plan that covers your allergy shots and other allergy medication you need.
The Wrong Test Can Be A Waste Of Money
Allergy tests can cost a lot. A skin allergy test can cost $60 to $300. A blood test can cost $200 to $1,000. A blood test for food allergies can cost hundreds of dollars, and testing for chronic hives can cost thousands of dollars. Your health insurance may not cover the costs of these tests. And without a doctors exam, the test may not even tell you what is causing your symptoms or how to treat them.
Also Check: Can Antibiotics Cause Itchy Skin
Are You Looking For Free Insurance Quotes
Secured with SHA-256 Encryption
|
D. Gilson is a writer and author of essays, poetry, and scholarship that explore the relationship between popular culture, literature, sexuality, and memoir. His latest book is Jesus Freak, with Will Stockton, part of Bloomsburys 33 1/3 Series. His other books include I Will Say This Exactly One Time and Crush. His first chapbook, Catch & Release, won the 2012 Robin Becker Prize from Seve… |
Written byD. Gilson, PhD Professor & Published Author |
|
Leslie Kasperowicz holds a BA in Social Sciences from the University of Winnipeg. She spent several years as a Farmers Insurance CSR, gaining a solid understanding of insurance products including home, life, auto, and commercial and working directly with insurance customers to understand their needs. She has since used that knowledge in her more than ten years as a writer, largely in the insuranc… |
Farmers CSR for 4 Years |
Will Medicare Pay For Treatment For A Detached Retina
A detached retina can cause permanent vision loss if not treated quickly. Medicare will cover surgery to repair a detached retina, but youll be responsible for your Part B deductible and 20 percent coinsurance, which Medigap can help take care of. Depending on where you have your procedure, a copayment might apply as well. Similarly, Medicare Advantage will pay for the cost of retina surgery to preserve vision.
Recommended Reading: Antibiotics Make You Itchy
Allergy Tests Without A Doctors Exam Usually Are Not Reliable
Many drugstores and supermarkets offer free screenings. And you can even buy kits to test for allergies yourself at home. But the results of these tests may be misleading.
- The tests may say you have an allergy when you do not. This is called a false positive.
- These free tests and home tests for food allergies are not always reliable.
License For Use Of Current Dental Terminology
End User License Agreement:These materials contain Current Dental Terminology , copyright © 2020 American Dental Association . All rights reserved. CDT is a trademark of the ADA.
The license granted herein is expressly conditioned upon your acceptance of all terms and conditions contained in this agreement. By clicking below on the button labeled I accept, you hereby acknowledge that you have read, understood and agreed to all terms and conditions set forth in this agreement.
If you do not agree with all terms and conditions set forth herein, click below on the button labeled I do not accept and exit from this computer screen.
If you are acting on behalf of an organization, you represent that you are authorized to act on behalf of such organization and that your acceptance of the terms of this agreement creates a legally enforceable obligation of the organization. As used herein, you and your refer to you and any organization on behalf of which you are acting.
Read Also: Can Allergies Cause Lost Voice
Does Medicare Cover Dry Eyes And Allergies
Though having dry eyes wont necessarily impact your vision, it can be a painful condition that affects your quality of life. Medicare will generally cover an exam to diagnose the problem since its not considered routine, at which point youll be on the hook for 20 percent coinsurance on top of your Part B deductible. Your Part D plan might also cover medication to treat the condition, though in some cases, over-the-counter treatment will suffice. Youll get similar coverage with a Medicare Advantage plan, and Medigap can help with your out-of-pocket costs.
How Does The Process Work
The first step is to confirm a patients allergies through allergy testing. Then, a custom-mixed vial of drops is prepared for the patient. The patient takes drops under the tongue daily. During the first four months, called the escalation phase, the dosage is gradually increased. After that, in the maintenance phase, the patient takes the same dose of drops each day.
Also Check: Celiac Swollen Lymph Nodes
Your Costs For Opdivo
Depending on the type and amount of Medicare coverage you have, you can expect to spend anywhere from zero dollars to as much as $2,670 per Opdivo infusion, according to Bristol-Myers Squibb Co., the manufacturer of Opdivo.
Bristol-Myers claims that more than 60 percent of patients paid $25 or less for each infusion in 2019.
Medigap and Medicare Advantage plans can greatly reduce your out-of-pocket costs. Check with your plan administrator about what your responsibility will be for your plan.
Your Costs For Immunotherapy With Medicare
You will still have to pay certain out-of-pocket costs for immunotherapy cancer treatment even if you are covered by Medicare.
Your Medicare Part B deductible applies. After meeting your deductible, you will also have to pay 20 percent of the Medicare-approved cost of your immunotherapy treatments.
Your Medicare Part A deductible will most likely be met if you complete all your necessary doctor visits and immunotherapy treatment sessions.
A Medigap policy may help cover some of your out-of-pocket costs if you have Original Medicare Medicare Part A and Part B. Medigap plans are sold by private insurers. Check with your plans administrator to find out exactly what costs you may still be responsible for paying.
Medicare Advantage plans are also sold by private insurers. They are required by law to cover everything Original Medicare covers. Medicare Advantage plans also have a maximum out-of-pocket limit that may save you money.
Check with your Medicare Advantage plan administrator to find out the specific benefits your plan offers and to see if your plan provides additional benefits above what Original Medicare will cover.
Also Check: Almond Extract Nut Allergy
Does Medicare Cover Xolair
Yes! 98% of Medicare Advantage plans and Medicare Part D plans cover Xolair.1
- Medicare Advantage plans that offer prescription drug coverage are called Medicare Advantage Prescription Drug Plans . Most Medicare Advantage beneficiaries are enrolled in MA-PDs.2
- Medicare prescription drugs plans each have their own formulary, or drug list, that details what prescription drugs are covered by the plan and how they are covered.
Drug coverage may vary based on plan availability. You may be able to find Medicare Advantage plan options in your area that cover Xolair.
Find Medicare Advantage plans with drug coverage
Or call 1-800-557-6059TTY Users: 711 24/7 to speak with a licensed insurance agent.
You can also compare Part D prescription drug plans available where you live and enroll in a Medicare prescription drug plan online when you visit MyRxPlans.com.
How Much Do Allergy Shots Cost
The cost of allergy shots can vary based on your plans coverage and out-of-pocket costs. Itll also depend on whether you meet Medicares eligibility requirements.
When starting treatment, youll typically get two shots per week for 6 months. There are two parts that factor into your costs:
- the allergen serum itself
- administration fees for the doctor and medical facility
Without insurance, shots may be $1,000 to $4,000 each year or higher when you first start treatment. During the maintenance phase, youll receive a shot once or twice per month for 3 to 5 years, so your costs will come down then.
Read Also: Robitussin Cold And Allergy
Skin Patch Testing For Irritable Bowel Syndrome
Tsai and associates stated that IBS is a chronic functional GI disorder afflicting a large number of people worldwide. These researchers carried out a population-based cohort analysis to examine the risk of IBS in children with atopic dermatitis as one of the first steps in the atopic march. From 2000 to 2007, a total of 120,014 children with newly diagnosed AD and 120,014 randomly selected non-AD controls were included in the study. By the end of 2008, incidences of IBS in both cohorts and the AD cohort to non-AD cohort HRs and CIs were measured. The incidence of IBS during the study period was 1.45-fold greater in the AD cohort than in the non-AD cohort . The AD to non-AD HR of IBS was greater for girls and children greater than or equal to 12 years . The HR of IBS in AD children increased from 0.84 for those with less than or equal to 3 AD-related visits to 16.7 for those with greater than 5 visits . The authors concluded that AD children had a greater risk of developing IBS further research is needed to clarify the role of allergy in the pathogenesis of IBS.
Cost Of Allergy Shots

The cost of allergy shots may vary depending on the coverage plan and incidental costs. It will also depend on if you meet the eligibility requirement of Medicare. When beginning treatment, you will generally receive two shots every week over six months. Your costs have two parts:
- Administrative fees for the physician and the medical center
- The allergy serum
Without insurance, shots can cost between $1,000 and $4,000 every year or more when treatment begins. At the maintenance phase, you will receive one or two shots per month for around 3-5 years to lower the costs at that time.
Also Check: Allergy Medicine Cetirizine
What Allergy Tests Does Medicare Cover
Medicare only covers specific types of allergy tests, and only when the tests have proven to provide effective and accurate results for certain types of allergens.
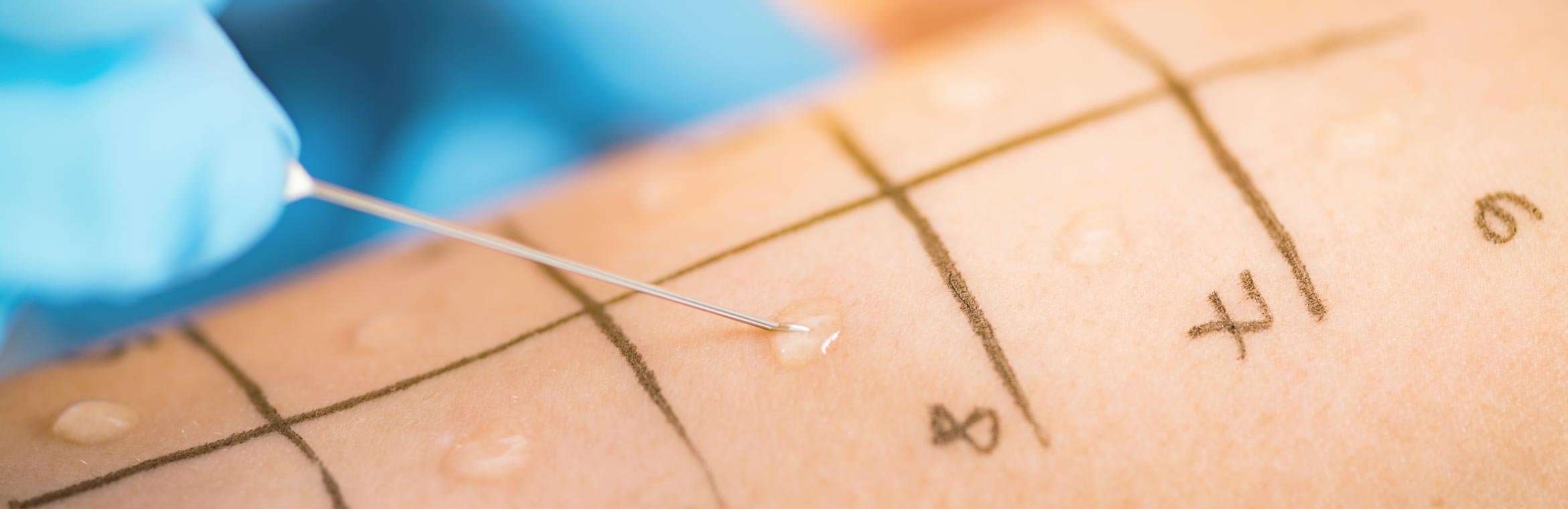
Skin tests that involve scratching, pricking or puncturing are the most common types of skin tests. Medicare covers these tests when IgE-mediated reactions occur to the following types of suspected allergens:
- Food
- Insects that sting
- Specific types of drugs, like penicillins
Intradermal, or intracutaneous testings, are tests that involve injecting a small amount of the allergen into your skin. Medicare covers these when the following types of suspected allergens cause IgE-mediated reactions occur:
- Inhalants
- Insects that sting
- Specific types of drugs
Medicare can also cover testing for food allergies used on an outpatient basis and deemed reasonable and necessary for the patient, according to the Medicare National Coverage Determinations Manual.
As always, Medicare coverage eligibility comes down to how necessary and reasonable the treatment is for you, as well as your particular Medicare plan. You should speak with a medical professional to determine if Medicare covers your particular allergy testing and/or allergy shots.

