Can A Flu Shot Make You Get Sick
It isnt out of the ordinary to react to the flu shot, as its simply a sign that your immune system getting to work protecting you. Common responses include a sore arm, headache, nausea, muscle aches or a mild fever. The vaccine itself is adapted every year, Dr. Ford says. So its very hard to predict, from one year to the next, if youre going to have a mild reaction, no reaction or a more problematic reaction.
However, if you do get sick after getting a flu shot, its not because of the vaccine. The only direct reactions to the shot are going to happen within the first 24 to 48 hours, Dr. Ford affirms. As mentioned before, if you get sick after that, people might think its related to getting the flu shot. But its just a coincidence.
Allergy Dos And Don’ts: Take A Sick Day
“What you don’t want to do is let allergies run your life,” says Anju Peters, MD, an allergy specialist in the division of allergy and immunology at Northwestern Memorial Hospital in Chicago. “I would never tell a patient with allergies to stay home from work unless they had an asthma exacerbation,” she adds. Instead, she says to investigate good allergy treatment options.
“If you have mild symptoms, try over-the-counter antihistamines, but stay away from the sedating ones,” Dr. Peters says. Instead, use non-sedating ones or try a saline rinse to wash allergens out of your nose.
How Well Do The Treatments Work
If you stick with allergy shots long enough, thereâs a good chance youâll see improvement or even an end to your allergy symptoms. About 85% of people with hay fever who get this type of treatment say their allergy symptoms get better.
âThatâs one of the things I find pretty neat as an allergist,â Wada says. âTypically, a lot of the treatments we have are geared toward treating the symptoms. This is one of the few things we have toward the root of the problem.â
Sublingual treatments havenât been studied as much as allergy shots. They havenât been shown to work as well as allergy shots. But if youâre up for the commitment of taking the medicine day in, day out, as prescribed, it might be an option to explore for the specific allergies it targets.
Show Sources
Read Also: Zurtech
How Long To I Have To Keep Getting My Allergy Shots
There are two phases to allergy shot therapy: a build-up phase and a maintenance phase.
- Build-up phase: In this phase you will start with a low dose injection and build to a higher dose of allergens over time. For typical immunotherapy this phase lasts from 6 to 10 months, depending on how often you get your shots and how well you tolerate them. The build-up phase for venom therapy generally lasts for 10 weeks.
- Maintenance phase: When you reach your effective therapeutic dose you will begin the maintenance phase. During this phase you receive your allergy shots less often, usually every 3 to 4 weeks. The maintenance phase typically lasts 3-5 years .
Allergy Shots: Could They Help Your Allergies
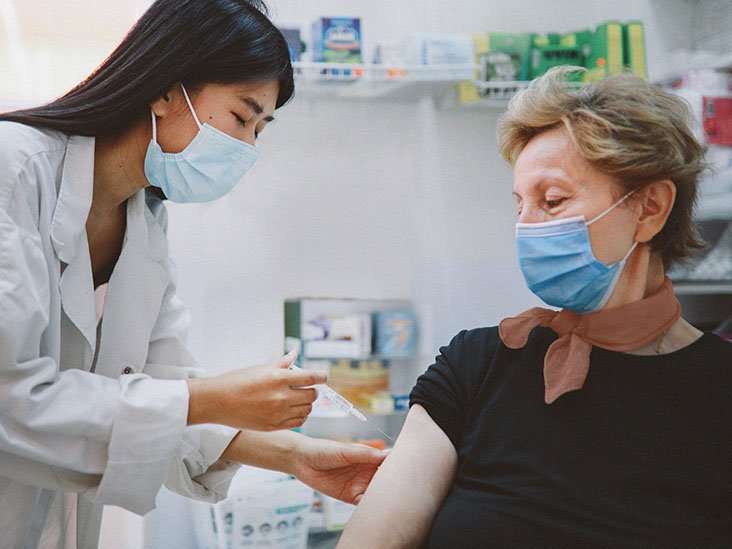
Another name for allergy shots is allergen immunotherapy. It is a type of treatment that relieves symptoms for people who have chronic allergies. Allergy shots contain small amounts of the thing you are allergic to, called an allergen. The first shot you get has a low amount of the allergen. The dose increases with each shot. Over time, this process helps your body fight the allergen. Your immune system creates antibodies to block its effect. The result is your allergy symptoms become less severe.
There are simple ways you can ease mild reactions to a bee sting and avoid getting stung again. Read More
Read Also: Health Symptoms Flushed Face After Eating
Why Are Allergy Shots Used
An allergy is when the body’s immune system overreacts to a usually harmless substance. Things that cause allergic reactions are called allergens. Common allergens include dust mites, molds, pollen, pets with fur or feathers, stinging insects, and foods.
The body reacts to the allergen by releasing chemicals, one of which is histamine. This release can cause symptoms such as wheezing, trouble breathing, coughing, a stuffy nose, and more. Some allergic reactions can be serious.
The best way to prevent or control allergy symptoms is to avoid allergens. Allergists look for causes of an allergic reaction with skin tests and blood tests. Based on the test results, they can recommend treatments, including medicines and ways to avoid allergens.
If these treatments don’t help, the allergist might recommend allergy shots.
/7what Happens When You Get Sick
When a person gets sick, it probably means that the body has been infested by an infectious germ or virus, meaning that the immune system is already in a compromised, stressed-out state, working hard to remove the germ.
Its common knowledge that a vaccine works the best when a person’s immunity is healthy, well-developed and stress-free.
Existing sickness, or at a time of sickness, when the immune system is already busy fighting out the virus would mean that there would be risks for the vaccine to work well, making many wonder if getting a COVID vaccine would be safe or not.
Not to forget, suffering from respiratory symptoms like cough, a fever could be doubly dangerous right now, since they are possible COVID symptoms as well. This is the only reason why some are being turned away from vaccination centres right now, because of the risk of infection spread.
You May Like: Claritin Medication
A Shot Isn’t Your Only Option
For people who hate shots or can’t keep up with their intensive schedule, sub-lingual therapy may be another option. This type of immunotherapy is delivered in daily tablets that dissolve under the tongue, and only the first few doses need to be taken with a doctor present.
Sub-lingual therapies are currently on the market for grass pollen and for ragweed pollen . Some allergy practices will also administer liquid drops under-the-tongue to treat other types of allergies, although these treatments are not FDA-approved.
To get our top stories delivered to your inbox, sign up for the Healthy Living newsletter
Covid Booster Shot 101
First off, make sure you’re eligible for a COVID vaccine booster. All U.S. adults age 18+ are eligible to receive a booster, according to the Centers for Disease Control and Prevention, as long as….
-
It’s been at least 6 months since you finished your initial mRNA vaccine series .
-
It’s been at least 2 months since you got your Johnson & Johnson/Janssen vaccine.
FYI, you’re allowed to mix and match vaccines, according to the CDC. So, even if you got Moderna for your first and second dose, if your pharmacy or doctor only has doses of the Pfizer booster shot, that’s totally fine. In fact, there’s some evidence showing that mixing and matching different vaccines may offer increased protection against COVID-19 infection, but more comprehensive research is still underway, so you shouldn’t necessarily seek out a different brand for your booster.
Also Check: Cetirizine Hydrochloride Zyrtec
Symptoms: What Does An Allergy Cough Feel Like
Allergy-related cough is typically a “dry” cough, meaning you probably won’t cough up any mucus or phlegm. It can become chronic, lasting for several weeks at a time. Coughing can occur with several different conditions and illnesses. You’ll likely see a specialist, such as an allergist, for specific testing to diagnose your allergies.
Although coughing occurs with a variety of medical conditions, allergy cough occurs with other allergy symptoms, including:
- Sneezing
- Fatigue
Can You Get A Covid
If youve had a severe allergic reaction to another vaccine or injectable medication or have experienced anaphylaxis from any cause you can still receive the COVID-19 vaccine. However, your vaccination should be followed by a 30-minute observation period in a setting where personnel, equipment and supplies are present to manage anaphylaxis.
Anaphylaxis commonly occurs within 30 minutes of exposure and would be unusual after 60 minutes, says Dr. Lang.
Also Check: Claritin Rx
They Can Improve Mental Health Too
It’s not just physical symptoms that can get better with allergy shots mental state can improve, as wellespecially if severe allergies have really taken a toll on your health and happiness.
This may be especially true for insect allergies, a condition that can cause serious distress and affect a person’s ability to enjoy the outdoors. One 2014 study found that patients with insect-venom allergies who received immunotherapy not only had a lower risk of anaphylaxis and death than those who didn’t, but also had lower anxiety and depression scores.
Why Do Allergies Occur
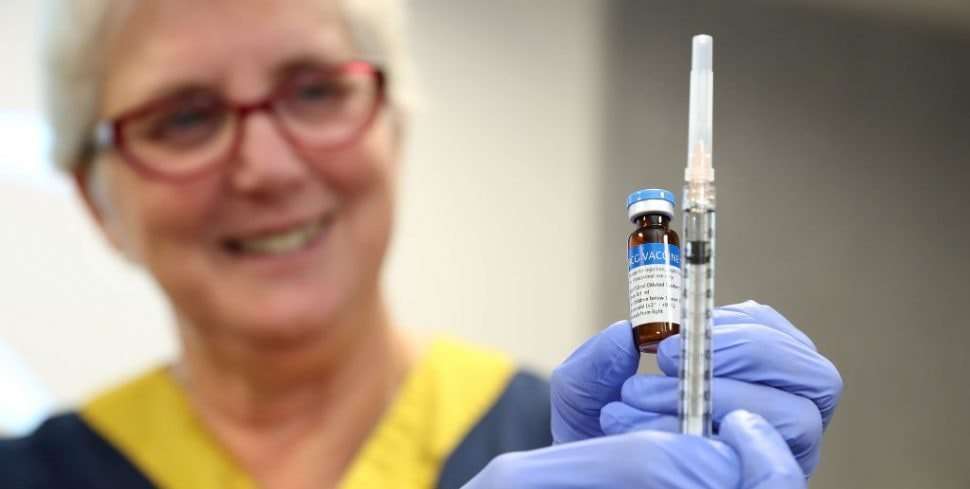
Your immune system is designed to identify and fight off illness-causing invaders, such as viruses. However, in the case of allergies, your body identifies certain substances such as pollen or pet dander as dangerous, though they arent.
Your immune system reacts to the substances which are called allergens and produces allergy symptoms, such as sneezing, watery eyes, and a runny nose.
Don’t Miss: Robitussin For Nasal Congestion
/7if You Have Already Had Covid
Another common misconception is that people who have recovered from coronavirus will not require a vaccine shot right now.
This is not true. Reinfection is a real possibility and there is strong evidence to suggest that immunity against COVID-19 may not be long-term for everyone. Getting a vaccine shot would mean that you double up your chances of protection and protect your fragile immune system.
Why It Is Done
Allergy shots can reduce your reaction to allergens, which can result in fewer or less severe symptoms. They may also prevent children who have allergic rhinitis from getting asthma.footnote 1 Recommendations on when to get allergy shots vary, but in general you and your doctor may consider them when:
- Allergy symptoms are severe enough that the benefit from the shots outweighs the expense and the time spent getting the shots.
- You are allergic to only a few substances, and they are hard to avoid.
- Avoiding allergens and using medicine do not control symptoms, or you have to take medicine all the time to control symptoms.
- Side effects of medicines are a problem.
- You want a treatment for the cause of your allergy, rather than treatment for just the symptoms.
- You have another condition that is being affected by allergic rhinitis, such as asthma.
- You want to lower the chance that you will develop asthma.
Also Check: Can Allergies Cause Swollen Lymph Nodes In Neck
Reasons To Avoid The Vaccine
Its recommended that if youve had an allergic reaction to any of the ingredients in the available vaccines, talk to your healthcare provider first. For instance, if youve had an allergic reaction to an ingredient in one of the mRNA vaccines , your provider might suggest Johnson & Johnsons COVID-19 vaccine. Or, if youre allergic to any ingredient in Johnson & Johnsons COVID-19 vaccine, your provider might recommend an mRNA vaccine. This can also apply if you had an allergic reaction to the first dose of a COVID-19 vaccine.
But having seasonal allergies or a shellfish allergy doesnt mean that you cant get vaccinated.
What Are Allergy Shots
Allergies are an overreaction by the immune system to a perceived threat. For years, oral antihistamine medications were the only treatment for allergies. Today, various treatments are available for allergies, including steroid nasal sprays, sublingual immunotherapy, and immunotherapy injections.
Allergy shots gradually retrain your immune system by injecting small doses of an allergy-containing solution. Over time, your sensitivity to the allergen decreases until your immune system is successfully desensitized to the allergen.
Immunotherapy in the form of allergy shots is effective, but you may feel hesitant due to prevailing myths surrounding this treatment. Here are the most common misconceptions and the facts you should know.
Recommended Reading: Pseudoephedrine Allergic Reaction
If The Omicron Variant Spreads Here Will Florida See More Lockdowns Mask Mandates Or Vaccinate Mandates
No, according to Governor Ron DeSantis, who said at an event in Oldsmar that there would be no further lockdowns or other restrictions because of the omicron variant.
A special session of the Florida Legislature, demanded by DeSantis to undermine the COVID safety measures for large businesses from the Biden administration and stop local governments and schools from enacting their own, produced four laws, which added more opt-out options from federal COVID rules and banned all government and school COVID-related mandates, with stiff fines for violations.
Are vaccine mandates banned in Florida now? What happened in the Legislative Special Session
How To Know Which Cold And Allergy Meds Are Safe
Check with your healthcare provider first if you’re breastfeeding and plan to take medication. Avoid taking unnecessary medications, such as herbal medications, high-dose vitamins, and unusual supplements.
Also, ask your doctor about timing. For instance, taking the medication immediately after breastfeeding might help minimize your baby’s exposure. However, different drugs peak in breast milk at different times.
Cold and allergy meds that are safe while breastfeeding include:
Some medications to avoid while breastfeeding include:
- Antihistamines, like Benadryl, have negative effects on breastfeeding and should be avoided if possible. Medicines like this decrease milk supply if used at high doses and for long periods of time.
- Sudafed can decrease milk supply and should also be avoided if possible.
Continued
Read Also: Can Seasonal Allergies Make You Throw Up
Should I Get A Flu Shot
Yes. Influenza is still a dangerous virus and flu shots, while not perfect, still help a great deal.
The Centers for Disease Control and Prevention recommend that, with rare exceptions, everyone 6 months and older get a flu vaccine every season. Public health experts say vaccination is vital to protect individuals, communities and to avoid burdening already overtaxed health care systems.
“The big risk here is that our healthcare system has limited capacity. In the winter, it usually hits that capacity in many places absent COVID, and flu is often a big contributor,” Dan Salmon, director of the Institute for Vaccine Safety and a professor in the Department of International Health at Hopkins University said during a press briefing.
If you are prone to catching the flu or colds, you may consider adapting some of the measures used to prevent COVID. Last year influenza virtually disappeared, in large part because of widespread adherence to COVID safety measures social distancing, mask-wearing and hand washing.
-
Wash your hands often with soap and water, or use hand sanitizer in a pinch.
-
Avoid crowds and poorly ventilated indoor spaces.
-
Stay 6 feet from people outside the home.
They’re Not Recommended For Everyone

Most adultsand children ages 5 and upcan get allergy shots. But if you or your child has severe, uncontrolled asthma, your doctor may recommend against them. “In our practice, if a patient’s asthma is flaring or even if they’re sick, we generally wait to give the shot until they’re feeling better,” says Dr. Dziadzio.
Women who become pregnant while in the maintenance phase of allergy shots can continue their treatment. But women shouldn’t start allergy shots for the first time, or increase their dosage, while pregnant.
Certain medicines, like beta blockers, can reduce the effectiveness of epinephrinethe lifesaving drug used to treat anaphylactic shock. Because anaphylaxis is a rare but serious risk for people getting allergy shots, they may not be recommended for people who take these drugs.
You May Like: Twix Peanuts
They Can Take A Few Years To Really Work
Allergy shots aren’t a quick fix: While some people may start to feel better during the build-up phase of their treatment, most people won’t experience noticeable improvement until they’ve been in the maintenance phase for six to 18 months, says Dr. Dziadzio.
In fact, a 2017 British study found that it took three full years for allergy shots for hay fever to be more effective than placebo shots. The maintenance phase for most allergy shots is usually continued for three to five years. Some patients experience long-lasting relief after that, and some may need continued treatment.
What Are The Symptoms For The Flu
More or less the same thing, except for the loss of taste or smell.
COVID-19 symptoms usually appear two to 14 days after exposure to the coronavirus. Influenza symptoms start to show up about one to four days after exposure to an influenza virus.
But COVID-19 can cause more serious illnesses in some people than the flu, as well as complications such as blood clots, lasting respiratory problems.
Do you have symptoms of the flu or COVID-19? Here is how you can tell the difference.
Recommended Reading: Does Twix Have Peanut Butter
Allergy Dos And Don’ts: Get Extra Rest
“The answer is a bit tricky,” says Novey. Resting doesn’t improve allergy symptoms because the problem is not caused by a weak immune system, which would be improved by rest. “Now,” he adds, “here’s the tricky part. Allergy symptoms make it easier to get an infection, like a sinus infection. If you are rested, you are less likely to have your allergy symptoms escalate into another type of infection.”
Myth: Allergy Shots Dont Really Work
Allergy shots are an effective and unique method of treating allergies. Immunotherapy changes the way your body responds to the environment so symptoms like sneezing and watery eyes decrease. Your allergy shot is formulated using a very small amount of all-natural protein extracts that, when given correctly, provides significant relief for most patients.
Also Check: Joint Pain Itchy Skin Fatigue
What If I’ve Had Covid Before Am I Immune Now
While previous infection helps your body fight off reinfection, it is still possible to get COVID again. And it may be even easier with omicron.
People infected longer ago with earlier variants are at higher risk of reinfection with omicron, South African studies have shown, with people infected in their first wave early last year having a 73% chance of reinfection. Those infected in its most recent delta wave have a 40% risk of reinfection with omicron, the new study showed.
A preliminary briefing released by the United Kingdom Friday showed an approximately three- to eight-fold increased risk of reinfection with the omicron variant.
‘It was just a matter of time’: How scientists in San Francisco found the first case of the omicron COVID-19 variant in the US

